Mental health care is a rapidly growing segment of the healthcare industry in the United States. As awareness increases and more patients seek therapy, counseling, and psychiatric care, providers face a major operational challenge: managing accurate billing for mental health services. Unlike general medical billing, mental health billing involves unique coding structures, compliance rules, payer policies, and documentation requirements.
For therapists, psychiatrists, psychologists, and behavioral health clinics, understanding how billing works is essential for maintaining financial stability and regulatory compliance. Errors in claims, incorrect coding, or delays in insurance processing can significantly impact revenue.
This guide explains how billing for mental health services works in the U.S., common challenges providers face, and how professional mental health billing services help improve efficiency and reimbursement.
Why Billing for Mental Health Services Is Complex
Mental health billing differs from traditional medical billing because services are often session-based, documentation-heavy, and governed by specialized codes.
Several factors contribute to this complexity:
Multiple CPT codes are used depending on session duration and therapy type
Insurance providers apply different policies for behavioral health coverage
Documentation requirements are stricter for therapy sessions
Prior authorization is often required for extended treatment plans
Medicare and Medicaid have unique guidelines for billing mental health
Because of these variables, many providers rely on professional billing services for mental health clinics to reduce claim denials and streamline reimbursement.
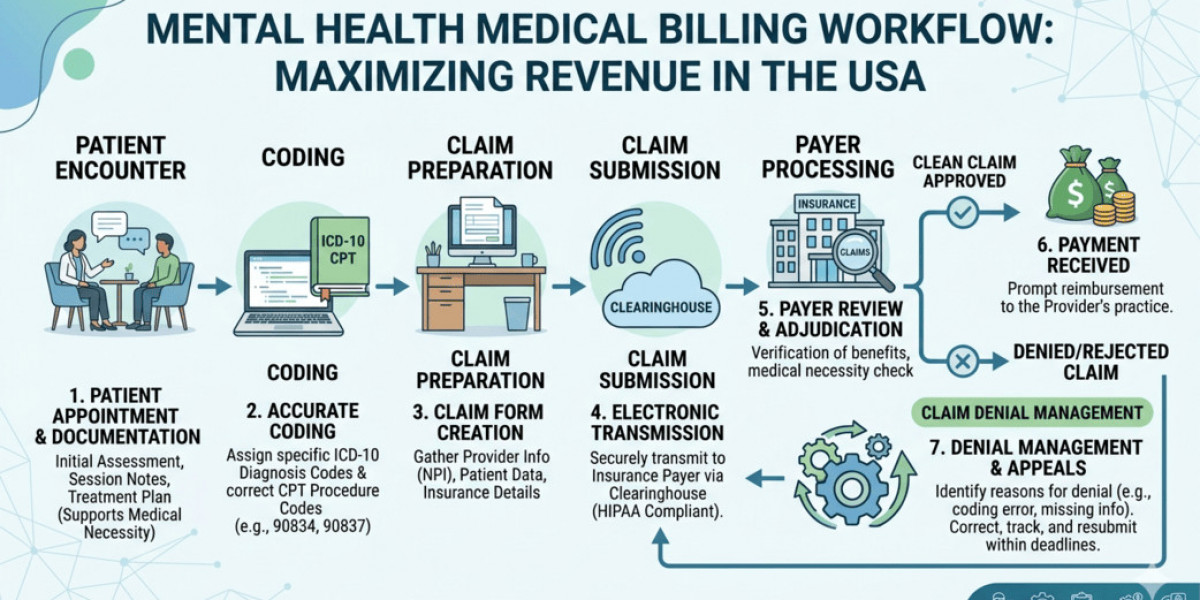
Understanding the Mental Health Billing Process
Billing mental health services follows a structured process similar to other medical specialties but with added attention to therapy documentation and coding accuracy.
Patient Insurance Verification
Before treatment begins, insurance eligibility must be verified. This step confirms coverage limits, co-payments, and authorization requirements for behavioral health services.Accurate Clinical Documentation
Therapists and psychiatrists must document session duration, treatment type, diagnosis codes, and therapeutic interventions.Coding and Claim Creation
Coding and billing for mental health services require precise CPT and ICD-10 coding. Even small errors can lead to claim rejection.Claim Submission
Claims are submitted electronically to insurance payers through clearinghouses.Payment Posting and Follow-Up
After processing, payments are posted and any denied claims are reviewed and resubmitted.
A reliable mental health billing company ensures every step of this workflow is managed efficiently to avoid delays.
Common CPT Codes Used in Mental Health Billing
Proper coding is essential in medical billing for mental health. Some of the commonly used CPT codes include:
90791 – Psychiatric diagnostic evaluation
90832 – Psychotherapy session (30 minutes)
90834 – Psychotherapy session (45 minutes)
90837 – Psychotherapy session (60 minutes)
90846 – Family psychotherapy without the patient present
90847 – Family psychotherapy with patient present
96127 – Brief emotional or behavioral assessment
Billing medicare for mental health services also requires careful adherence to these codes along with Medicare-specific documentation standards.
Key Challenges in Mental Health Billing
Even experienced providers often struggle with billing mental health services due to industry-specific complications.
Insurance Policy Variations
Different insurance carriers follow unique policies regarding therapy sessions, telehealth coverage, and reimbursement limits.
High Claim Denial Rates
Improper coding or incomplete documentation can lead to frequent denials, especially in behavioral and mental health billing services.
Authorization Requirements
Many payers require prior authorization for long-term therapy or psychiatric treatment.
Credentialing Issues
Providers must be properly enrolled with insurance networks before submitting claims. Mental health billing and credentialing services help address this challenge.
Session-Based Billing
Unlike procedural medicine, therapy sessions depend heavily on accurate time tracking and session documentation.
Because of these obstacles, many clinics turn to outsourced billing for mental health to improve operational efficiency.
Benefits of Outsourcing Mental Health Billing
Outsourcing mental health billing has become a common strategy for therapists, counseling centers, and behavioral health clinics seeking to improve revenue cycle performance.
Access to Industry Experts
Mental health billing specialist companies understand payer rules, coding requirements, and regulatory guidelines specific to behavioral healthcare.
Reduced Administrative Workload
Therapists can focus on patient care while billing companies for mental health handle claim submissions, follow-ups, and payment posting.
Faster Reimbursement
Professional mental health billing solutions reduce claim errors and speed up insurance processing.
Improved Revenue Cycle Performance
Outsourcing mental health billing and coding helps clinics identify billing gaps and recover lost revenue.
Scalability for Growing Practices
As clinics expand, outsourcing allows them to manage larger patient volumes without hiring additional administrative staff.
For these reasons, many providers partner with a mental health billing services company that specializes in behavioral healthcare.
How to Choose the Right Mental Health Billing Company
Selecting the right billing partner can significantly impact the financial health of a practice.
Industry Specialization
Look for a top mental health billing company that has direct experience working with therapy practices, psychiatrists, and behavioral health clinics.
Credentialing Support
Providers benefit from mental health billing and credentialing services that ensure enrollment with major insurance networks.
Compliance Expertise
The best mental health billing services company stays updated with HIPAA regulations, payer updates, and coding changes.
Transparent Reporting
A good mental health medical billing provider offers clear revenue reports and claim tracking systems.
Technology Integration
Efficient billing companies integrate with EHR and practice management systems to simplify workflow.
Many clinics compare several mental health billing specialist companies before selecting the best mental health billing company for their needs.
Mental Health Billing for Different Provider Types
Billing requirements vary depending on the type of mental health professional.
Psychiatrists
Psychiatrists often bill both evaluation and medication management services. Their billing includes psychotherapy codes combined with medical evaluation codes.
Psychologists
Psychologists primarily bill psychotherapy sessions and psychological testing services.
Licensed Therapists and Counselors
Billing for mental health therapists typically involves time-based psychotherapy CPT codes and treatment documentation.
Group Therapy Practices
Clinics with multiple therapists benefit from outsourced billing for mental health that manages claims across providers and payers.
Each provider type requires specialized billing services for mental health providers to ensure accurate claims processing.
Technology and Automation in Mental Health Billing
Modern technology has significantly improved billing for mental health services.
Electronic Health Records Integration
EHR systems automatically link clinical notes with billing codes.
Automated Eligibility Verification
Insurance verification tools help reduce claim denials.
Analytics and Revenue Reporting
Advanced billing platforms track claim performance and identify reimbursement trends.
Telehealth Billing Support
With the growth of virtual therapy, billing for mental health services now includes telehealth coding and payer-specific guidelines.
These innovations help mental health billing services deliver faster and more accurate claim processing.
Cost Considerations When Outsourcing Billing
Pricing models vary across billing providers.
Most billing companies charge based on a percentage of collected revenue, typically between 4 percent and 10 percent.
Some providers search for a cheap outsource mental health billing company to reduce costs. However, focusing only on price may result in poor claim management or compliance risks.
Instead, practices should evaluate the value offered by the best outsource mental health billing and coding services in terms of expertise, denial management, and revenue improvement.
A reliable mental health billing company ultimately generates higher collections that outweigh service fees.
Future Trends in Mental Health Billing
The behavioral healthcare sector is expected to continue expanding in the United States.
Key trends shaping the future of mental health billing include:
Increased teletherapy and digital mental health services
Expanded insurance coverage for behavioral healthcare
AI-driven claim review and billing automation
Greater regulatory oversight and compliance requirements
As the industry evolves, billing services for mental health clinics will play an increasingly critical role in maintaining operational efficiency.
Conclusion
Billing for mental health services is far more complex than traditional medical billing due to specialized therapy codes, payer regulations, and documentation standards. Providers must navigate insurance verification, accurate coding, claims submission, and denial management while focusing on patient care.
Working with experienced behavioral & mental health billing services helps providers reduce administrative burden, minimize claim errors, and improve reimbursement rates. Professional mental health billing solutions ensure that therapists, psychiatrists, and counseling practices can operate efficiently while maintaining compliance with healthcare regulations.
Healthcare organizations seeking reliable revenue cycle support often partner with experienced providers like 247 Medical Billing Services, which offers comprehensive medical billing services, medical coding services, medical billing and coding services, revenue cycle management, and credentialing services to help healthcare practices strengthen their financial performance.
Frequently Asked Questions
What is billing for mental health services?
Billing for mental health services refers to the process of documenting therapy or psychiatric treatment, assigning appropriate CPT and diagnosis codes, submitting insurance claims, and managing reimbursement for behavioral healthcare services.
Why do mental health providers outsource billing?
Many providers choose outsourcing mental health billing to reduce administrative workload, improve claim accuracy, and ensure compliance with insurance regulations.
What services do mental health billing companies provide?
A mental health billing services company typically handles insurance verification, coding, claim submission, denial management, payment posting, and revenue cycle reporting.
How does Medicare billing work for mental health services?
Billing Medicare for mental health services requires specific CPT codes, proper documentation of therapy sessions, and adherence to Medicare coverage guidelines.
What should providers look for in the best mental health billing services?
Providers should evaluate experience in behavioral health billing, compliance expertise, transparent reporting, credentialing support, and integration with EHR systems when selecting the best mental health billing services.
Can small therapy practices benefit from outsourced billing?
Yes. Even small practices benefit from outsourced billing for mental health because it reduces administrative tasks, improves reimbursement rates, and allows therapists to focus more on patient care.